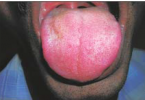
1. Herpetic Stomatitis
Clinical features
– Incubation period is 3-7 days.
– Mouth ulcers: multiple vesicles and round scattered ulcers with yellow slough
and erythematous halo; ulcers fuse to produce irregular lesions.
– Gingivitis: diffuse erythema and oedema, occasionally haemorrhagic.
– Cervical lymphadenitis.
– Fever.
– Malaise, irritability and anorexia.
Incidence
– Common cause of mouth ulcers in poor areas, with fever in children.
– It is also seen in adults, especially in more affluent communities.
Aetiology
– Herpes simplex virus (HSV), usually type 1.
Diagnosis
– Differentiate from other causes of mouth ulcers, especially hand, foot and mouth disease, chickenpox and shingles, herpangina, erythema multiforme and leukaemia.
– Smear for viraldamaged cells or immunostaining.
– Viral culture or electron microscopy is used occasionally.
– A rising titre of antibodies is confirmatory.
Management
– Soft diet and adequate fluid intake, antipyretics/ analgesics (paracetamol/acetaminophen elixir), local antiseptics (0.2% aqueous chlorhexidine mouthwashes), aciclovir orally or
parenterally in immunocompromised patients.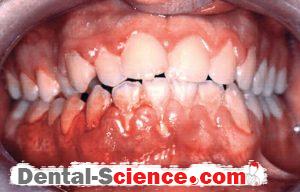

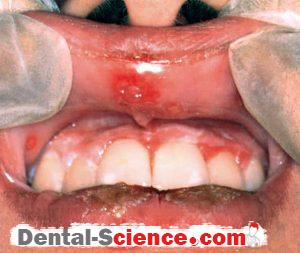
2. Herpes Labialis
Clinical features
– Prodromal paraesthesia or irritation. Erythema, then vesicles at/near
mucocutaneous junction of lip.
– Heals in 7-10 days.
Incidence
– Common, especially in immunocompromised.
Aetiology
– Herpes simplex virus (HSV), usually type 1.
– HSV latent in trigeminal ganglion is reactivated by sun, trauma, menstruation, fever,
HIV disease, immunosuppression, etc.
Diagnosis
– Viral damage can be confirmed by smear.
– Differentiate from zoster, impetigo or (rarely) carcinoma.
Management
– Penciclovir 1% cream or aciclovir 5% cream applied in prodrome.
– Immunocompromised may need systemic aciclovir (oral or i.v.).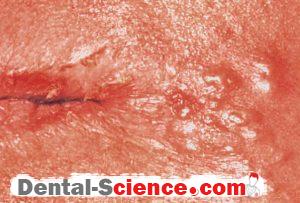
3. Recurrent intra-oral herpes
Clinical features
– Localised area of unilateral vesiculation followed by ulceration (erosion).
Incidence
– Rare.
Diagnosis
– Viral damage can be confirmed by smear.
– Differentiate from zoster or herpetiform ulcers (recurrent herpes is monolateral).
Management
– Aciclovir: 5% cream applied in prodrome.
– Immunocompromised patients may need systemic aciclovir (oral or i.v.), famciclovir
or valaciclovir.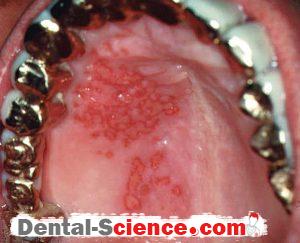
ــــــــــــــــــــ► ⒹⒺⓃⓉⒶⓁ–ⓈⒸⒾⒺⓝⓒⒺ ◄ــــــــــــــــــــ